The New Hospital Programme promises more efficient delivery through industrialisation. Kristina Smith speaks to programme leads from the NHS, Mace and Turner & Townsend

In February 2025, a group of 10 companies led by Mace and Turner & Townsend – the Health Delivery Partnership consortium – was appointed as the programme delivery partner for the New Hospital Programme (NHP).
The £50bn-plus programme will see 46 major hospital projects delivered between 2020, when the NHP was launched by the previous Conservative government, and the early 2040s.
Evolving as it progresses, with a Labour government ‘reset’ in January 2025, the NHP promises a new approach to hospital delivery. Rather than each NHS Trust doing their own thing as a client, there is to be an ‘industrialised’ approach – dubbed Hospital 2.0 – covering everything from business cases to bathroom pods.
Some six months after the programme delivery partner started work, CM caught up with three of the programme’s leaders to get a feel for what this new way of working might look like.

“The commercial model has been set up in order to make it attractive, to balance risks sensibly.”
Darren Colderwood is programme director and commission lead for the Health Delivery Partnership consortium; Darren Laybourn, global health lead at Turner & Townsend, is head of estimating, cost management and data tools and policies; and Doug Baldock is executive technical services director at NHP, responsible for design, sustainability, industrialisation and digital.
With seven of the 46 hospitals already built and others under way (see box), the remainder will be delivered under the new regime. Tier 1 contractors will become part of the Hospital 2.0 Alliance (H2A); 16 were shortlisted in June 2025 with dialogue underway to allocate the first 10 projects among them.
The plan is that the alliance model, based on the Institution of Civil Engineers’ Project 13, will be far less risky for contractors. “The commercial model has been set up in order to make it attractive, to balance risks sensibly; that’s a big factor in getting this up and running,” says Colderwood.
So far, that approach appears to be paying off. “We’ve attracted back into the market a significant number of contractors who had left because the risk was too great for them,” says Baldock.

The ultimate goal is better outcomes for patients. Myriad stakeholders including NHS clinicians, patient groups, various Royal Colleges, national clinical directors and NHS Estates have all fed into this standardised approach, which aims to see optimised hospital layouts, enabled by digital technologies and assembled using several standardised components such as MEP modules, pods and cladding.
Getting to this point will require a huge shift for the NHS Trusts, as well as for the construction supply chains delivering the programme. The idea is that working within the Hospital 2.0 blueprint will see tested and approved products and layouts deployed on every scheme, reducing risk and creating economies of scale. Getting Trusts to stick to that blueprint is vital, says Laybourn. “Hospital 2.0 is the DNA of the programme. If you break the DNA, the whole code falls down.”
Five years on
When the then-prime minister Boris Johnson announced NHP in 2020, the headline claims were that £20bn would be spent to build 40 hospitals by 2030. Interim delivery partner Mott MacDonald and interim commercial partner KPMG were appointed in 2021 and started working on a standardised approach, which would favour modern methods of construction and lead to economies of scale.
When the Labour government came into power, it ordered a strategic review of the NHP. Discussions with HM Treasury followed. As a result, hospitals containing reinforced autoclaved aerated concrete (RAAC) were prioritised, others were pushed back and delivery of the programme was organised into five-year waves, stretching out to 2040. Each wave is to be allocated £15bn of funding under the programme.

“There is a desire to cut the cost to get to the optimum level. At the same time, we want to increase predictability and reduce uncertainty.”
“In January, there was a reset which focused on establishing a credible and realistic time frame for delivery of all the schemes in the NHP,” explains Baldock. “With funding confirmed for the programme at that time – in waves aligned with spending reviews in each five-year period – the team has been establishing a schedule of area aligned to a cost plan for each scheme.”
At the time of the January 2025 reset, seven schemes – now dubbed Wave 0 – were under construction and six projects – Wave 1c – were under way, let under the previous ProCure 23 framework. Wave 1a, the RAAC hospitals and three more under Wave 1b will be let through H2A.
One of the biggest tasks for Laybourn and his team has been getting to grips with costs, pinning down areas, budgets and timeframes. Back in 2021, Mott Macdonald reported that there was a goal of 20% reduction in cost and 25% reduction in time. Today, NHP is being rather more cautious about such goals.
“There is a desire to cut the cost to get to the optimum level. As a programme we are not stating a particular percentage,” says Laybourn. “Working with alliance partners and all the supply chain will allow us to establish what the optimum time is within target envelopes. At the same time, we want to increase predictability and reduce uncertainty.”
New expertise
In addition to working on costing and procurement, the programme delivery partner has been getting up to speed with the other elements of the programme, including setting up processes and its team.
As well as regular construction players, the Health Delivery Partnership consortium has a couple of less conventional members too: beneath Mace and Turner & Townsend, Deloitte, Unipart and Amentum sit alongside Mott MacDonald, which leads a design team of WSP, HDR, KHS and specialist healthcare designer MJ Medical.
“If you look at the scope of work and the breadth of the scope we were asked to undertake, it is very, very broad,” says Colderwood. “It is broader than the scope that the previous interim delivery partner and the interim commercial partner covered.”
Deloitte is there for its experience in transformation, Unipart brings logistics and industrialisation expertise and Amentum is adding project management depth, says Colderwood. Having Mott MacDonald in the consortium creates continuity with the initial phases of the programme.
“Having a team with that many component parts is interesting to manage, but that’s my job,” says Colderwood.
Design work has been progressing on prototypes, says Baldock, to tie down details for any aspect that is novel or different from current standards. Offsite specialist Reds10 built a prototype ensuite patient room in its manufacturing facility in Driffield, East Yorkshire, to iron out issues such as coordination of services, clinical space around the bed, installation and maintenance space for services and constructability. All the hospitals will have individual, ensuite rooms.
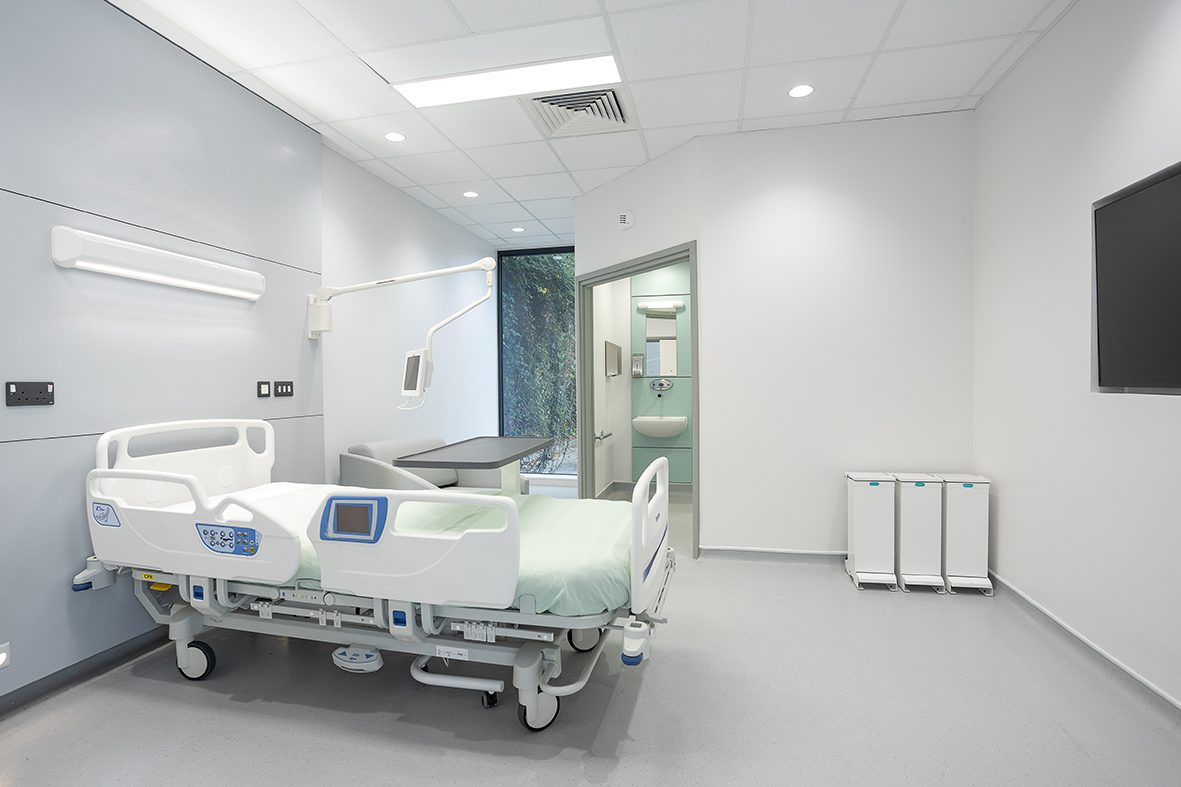
“This has been a huge help, not just for technical reasons but for clinical reasons to validate our design,” says Baldock. “We are doing a series of these over the next few years, way ahead of construction, so that we derisk the programme significantly before we get to any scheme, which is fairly novel in the NHS.”
The NHP will also use a toolkit of standardised parts aimed to bring economies of scale. There are currently seven standardised components: in-room MEP modules; horizontal MEP distribution modules; risers; ensuite bathrooms; facades; partitions; and doors.
It has been reported that the NHP is aiming for 80% standardisation. But that isn’t quite right, says Laybourn. “This isn’t only about building more offsite, it’s about industrialisation. We are aiming for 80% industrialised. We want to drive repeatability to our advantage.”
That repeatability extends to processes too, says Baldock. “We don’t want to restrict it to just focus on products. There are business cases that are quite unwieldy. Streamlining business cases is reducing costs.”
Holding the line
The first projects to test the industrialisation scenario will be Wave 1a, the seven RAAC hospitals which will start on site in late 2027 or early 2028. For Hospital 2.0 to work, it is vital that, in designing their hospitals, the NHS Trusts stick to the industrialised approach and the standardised components.
Already there is tension in this area, says Baldock. “The biggest challenge is getting them [the trusts] to hold the line so that when they get to RIBA stages 3 and 4, we can embed the products.”
Architects and designers working with the trusts are feeding back on how well the Hospital 2.0 methodology is being deployed on each scheme so that support can be given where necessary to keep trusts on track, says Baldock.
In parallel with developing the designs for Wave 1a, the team is also looking to optimise Wave 1c, the projects procured under the previous framework. “We are looking at how we can adapt certain aspects of Hospital 2.0, for example standardisation of room sizes and more modular construction,” says Laybourn. “Or, if they are in far-flung parts of the country, we are looking at how we can remove capacity issues and, at the same time, provide additional commercial support.”

“The biggest challenge is getting the trusts to hold the line so that when they get to RIBA stages 3 and 4, we can embed the products.”
Relationships established at this point could be important for the programme further down the line, says Laybourn. “We are trying to evolve the standing of the programme by showing the right behaviours on those projects. Those partners could be potential alliance partners.”
It’s not clear yet how far down the supply chain the alliance approach will be extended. Since competitive dialogue with the shortlisted contractors is still ongoing, this wasn’t something that Colderwood or Laybourn would discuss. A suppliers’ guide on the NHP website says that the alliance partners – tier 1 contractors – will “determine the optimal way of packaging and delivering their works, dependent on the scheme and their own delivery model”.
Some suppliers will work only within their region, whereas others might stretch across multiple regions, says Laybourn.
One of the most important tasks for the programme delivery partner will be ensuring that supply chain members are not overstretched or the market overheated, says Baldock. A programme intelligence portal (PIP) has been developed to aggregate all the components needed across all the projects in the programme to help manage this.

The NHP recognises there will be skills shortages in certain areas. Calderwood pinpoints the East of England where programmes such as Anglian Water’s AMP8 programme of works and Sizewell C will be competing with hospital builds. The NHP will be launching a skills academy at an event in November in a bid to train and upskill the supply chain.
In another six months, there will be a lot more to say, says Calderwood. But for now, it’s about getting the foundations and behaviours in place, so that the NHP isn’t just business-as-usual contracting.
“It’s not just about the number we are building in the next few years, it’s about setting a new standard and setting a new bar,” says Laybourn. “We are going through some hard yards, but we know those hard yards will prove fruitful for the long-term sustainable future of the NHS and its assets. For me, that’s what this programme really drives towards.”
The New Hospital Programme projects
Already completed (opened between 2021 and 2024)
- Hospital Northern Centre for Cancer Care
- Royal Liverpool Hospital
- Sycamore Unit at Northgate Hospital
- Brighton 3Ts Phase 1
- Greater Manchester Trauma Hospital
- Dyson cancer Care
- Midland Metropoliotan University Hospital
Wave 0 – under way
- Alumhurst Road Children’s Mental Health Unit, Dorset (Kier Construction)
- Royal Bournemouth Hospital, Dorset (Integrated Health Projects (Vinci-Sir Robert McAlpine))
- St Ann’s Hospital, Dorset (Kier Construction)
- Dorset County Hospital, Dorchester (Tilbury Douglas)
- CEDAR Programme (Sir Robert McAlpine)
- Oriel Eye Hospital (Bougues (UK))
- National Rehabilitation Centre (Integrated Health Projects)
Wave 1a – RAAC hospitals (to be delivered through Hospital 2.0 Alliance)
- West Suffolk Hospital, Bury St Edmunds (RAAC) £1 billion to £1.5 billion
- Hinchingbrooke Hospital (RAAC) £501 million to £1 billion
- James Paget Hospital, Great Yarmouth (RAAC) £1 billion to £1.5 billion
- Queen Elizabeth Hospital, King’s Lynn (RAAC) £1 billion to £1.5 billion
- Leighton Hospital (RAAC) £1 billion to £1.5 billion
- Airedale General Hospital (RAAC) £1 billion to £1.5 billion
- Frimley Park Hospital (RAAC) £1 billion to £2 billion
Wave 1b (to be delivered through Hospital 2.0 Alliance)
- Milton Keynes Hospital £500 million or less
- Hillingdon Hospital, north-west London £1 billion to £1.5 billion
- North Manchester General Hospital £1 billion to £1.5 billion
Wave 1c (more developed schemes, being delivered under ProCure 13)
- Poole Hospital, Dorset (integrated Health Projects) £500 million or less
- Derriford Emergency Care Hospital, Plymouth (Mace-Willmott Dixon) £500 million or less
- Cambridge Cancer Research Hospital (Laing O’Rourke) £500 million or less
- Shotley Bridge community Hospital, Durham (Tilbury Dougals) £500 million or less
- Women and Children’s Hospital, Cornwall (not yet awarded) £500 million or less
- Brighton 3Ts Hospital (Laing O’Rourke) £500 million or less
Wave 2
- Leeds General Infirmary £1.5 billion to £2 billion
- Specialist Emergency Care Hospital, Sutton £1.5 billion to £2 billion
- Whipps Cross University Hospital, north-east London £1 billion to £1.5 billion
- Princess Alexandra Hospital, Harlow £1.5 billion to £2 billion
- Watford General Hospital £1.5 billion to £2 billion
- Leicester Royal Infirmary, Leicester General Hospital and Glenfield Hospital £1 billion to £1.5 billion
- Kettering General Hospital £1 billion to £1.5 billion
- Musgrove Park Hospital, Taunton £501 million to £1 billion
- Torbay Hospital £501 million to £1 billion
Wave 3
- Charing Cross Hospital and Hammersmith Hospital, London £1.5 billion to £2 billion
- North Devon District Hospital, Barnstaple £1 billion to £1.5 billion
- Royal Lancaster Infirmary £1 billion to £1.5 billion
- St Mary’s Hospital, north-west London £2 billion or more
- Royal Preston Hospital £2 billion or more
- Queen’s Medical Centre and Nottingham City Hospital £2 billion or more
- Royal Berkshire Hospital, Reading £2 billion or more
- Hampshire Hospitals £2 billion or more
- Eastbourne District General, Conquest Hospital and Bexhill Community Hospital £1.5 billion to £2 billion
Comments
Comments are closed.











Having worked for a major main contractor I have serious doubts concerning the industry ability to deliver the programme to schedule. Being practical the odds of delivering all 46 hospitals to programme is zero, directly inpacting on the schedule for the later follow on schemes.